If the history of medical innovation has taught us anything, the technology that will replace the traditional screening mammogram has most likely already been invented. You just can’t expect that anyone will recommend it to you, nor should you expect insurance to cover it. Years of clinical study and millions of dollars will be needed to verify the results, convince referring doctors and assure insurance coverage.
And, if you think that hospitals, imaging centers and all breast experts will enthusiastically and rapidly embrace the new technology when mammography’s replacement is clinically proven, you’d be sadly mistaken. There is up to a 17 year lag in the adoption of new medical devices, even when they are clinically proven.(1)
If you were to ask most doctors their opinion of the best breast cancer screening tool, most would say—without hesitation—the mammogram. They say this because they have been told that mammography is the only screening technology that has been proven to save lives in numerous clinical studies. But that doesn’t mean other screening technologies aren’t going to be shown to be better at saving lives… or shown to provide superior detection when used in conjunction with mammography. Other technologies just aren’t yet supported by as many clinical studies as the mammogram, which is now a 40 year-old technology. Clinical studies are extremely expensive and take much time, but we are able to evaluate their promise based on the few studies that are available or in progress, practitioner experience with the technology and a little bit of common sense.
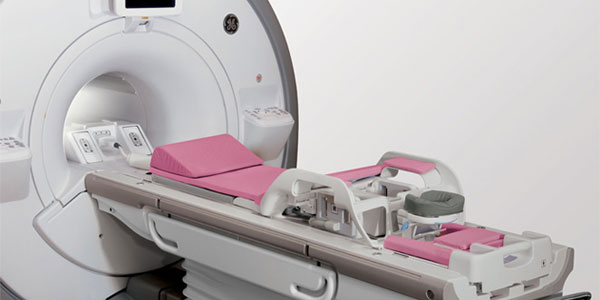
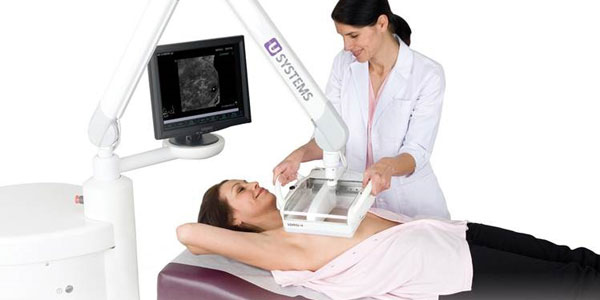
Here are the technologies that are either challenging the traditional mammogram as the gold standard, or that are used in conjunction with mammography to provide a greater chance for early detection and/or improve diagnostic capabilities: